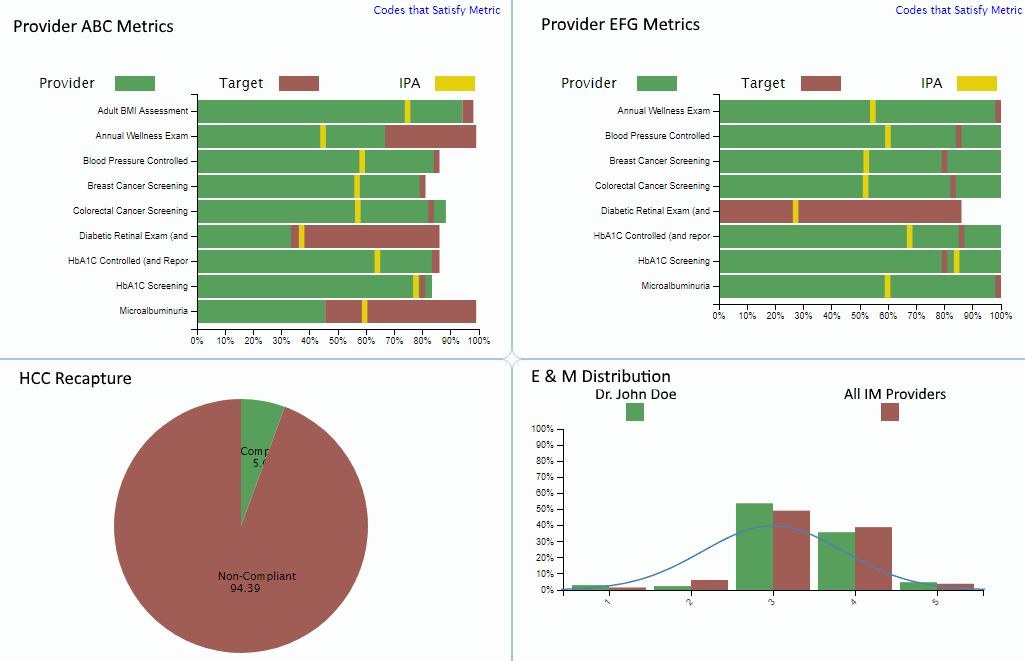
Utilization Dashboard
As more heathcare services are moving to a managed care system, the value of your data, and visibility to that data becomes more important than ever. Our custom dashboard software can handle multiple organizations at once and aggregates data for a management view, yet gives individual providers access as well. Providers are able to compare utilization numbers with their peers in a certain office or specialty, but remain anonymous otherwise.
These management systems are ideal for organizations in charge of patient care for a large set of members, such as physician associations and ACO's. We can provide a platform for risk management that uses existing claims data to help identify areas in need of improvement.
Live Patient Quality Metrics
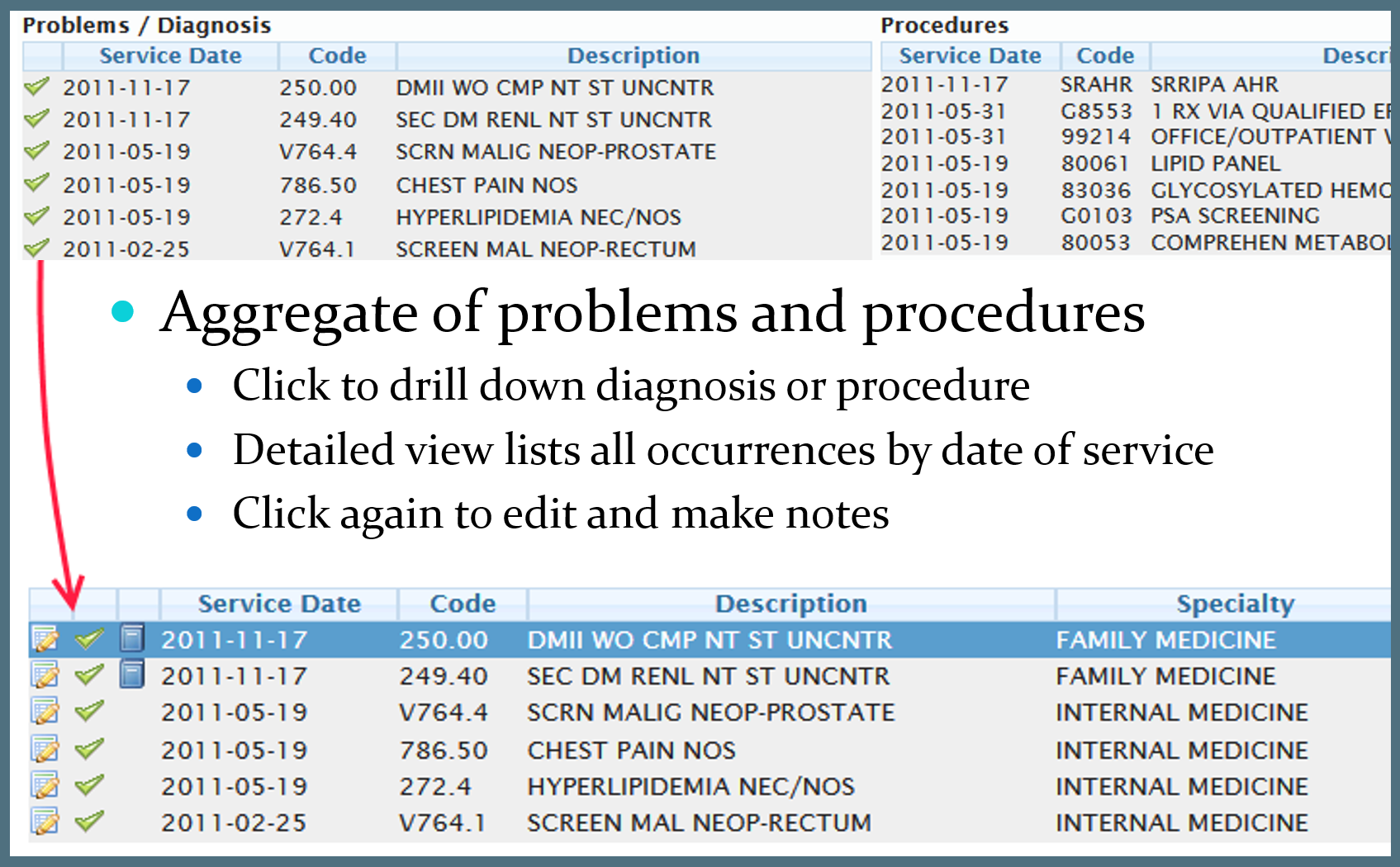
Primary Care Providers (PCP) in charge of patient overall health can track progress using an aggregated summary of all the patient's data. Claims and lab data from various sources are accumulated and sorted for ease of access. Procedures, diagnoses, encounters, prescriptions, and compliance metrics can all be drilled-down on to provide detail and make notes.
Patient alerts are listed here as well and give providers the ability to see the quality of care for each patient. If, for example, a diabetic patient is overdue for a eye exam, this report will alert the PCP and provide the date of the last exam.
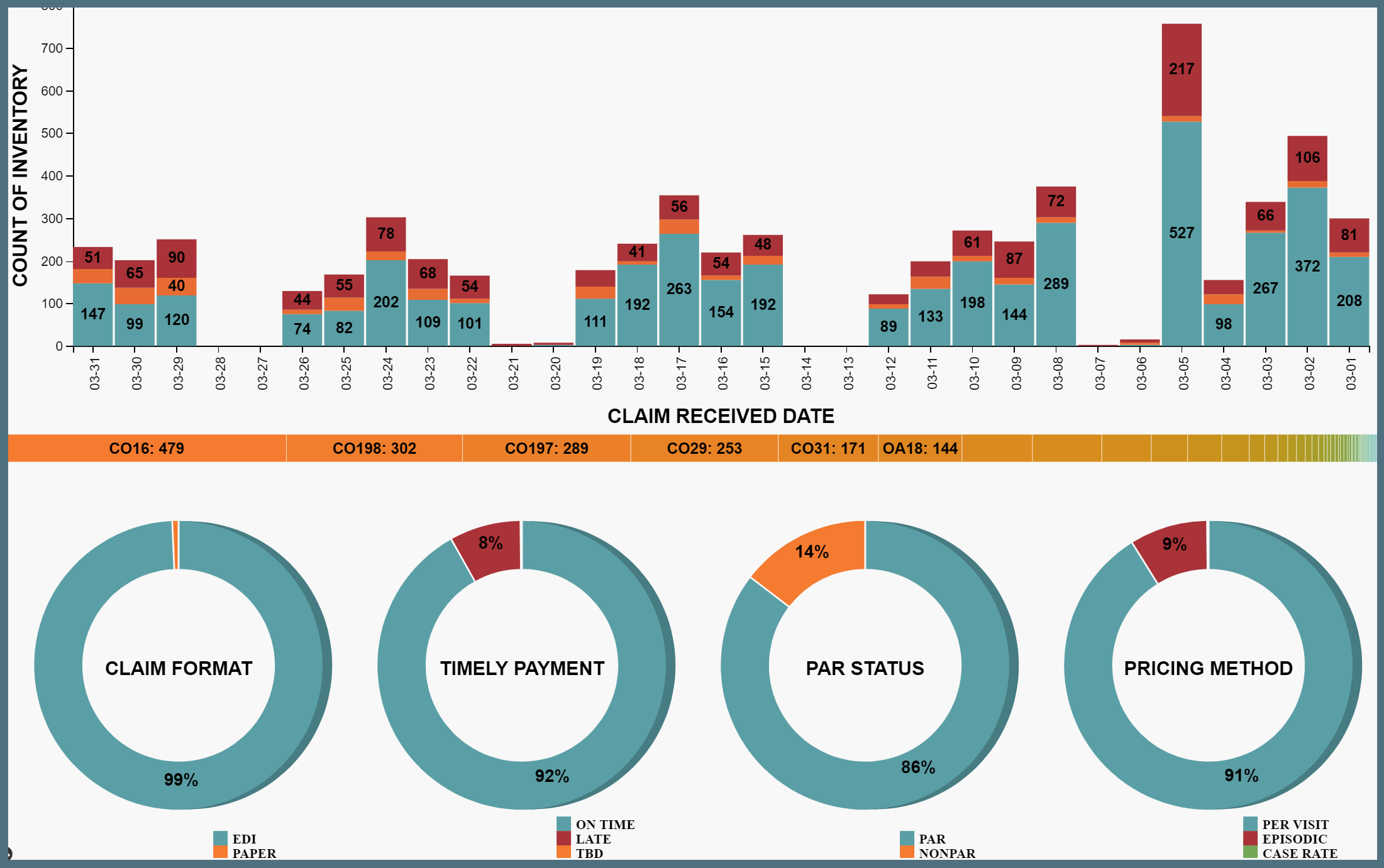
Data Warehouse
Provident Solutions has experience creating and maintaining patient care systems. These systems help you manage your patients and claims data. The goal is to create a standard framework that addresses the various requirements of the health plan.
Members with certain conditions that require care can be brought to your attention with a patient priority system. If your health plan is evaluating your organization on these conditions and cases, we can help you meet these metrics with your claims data and our reporting software.
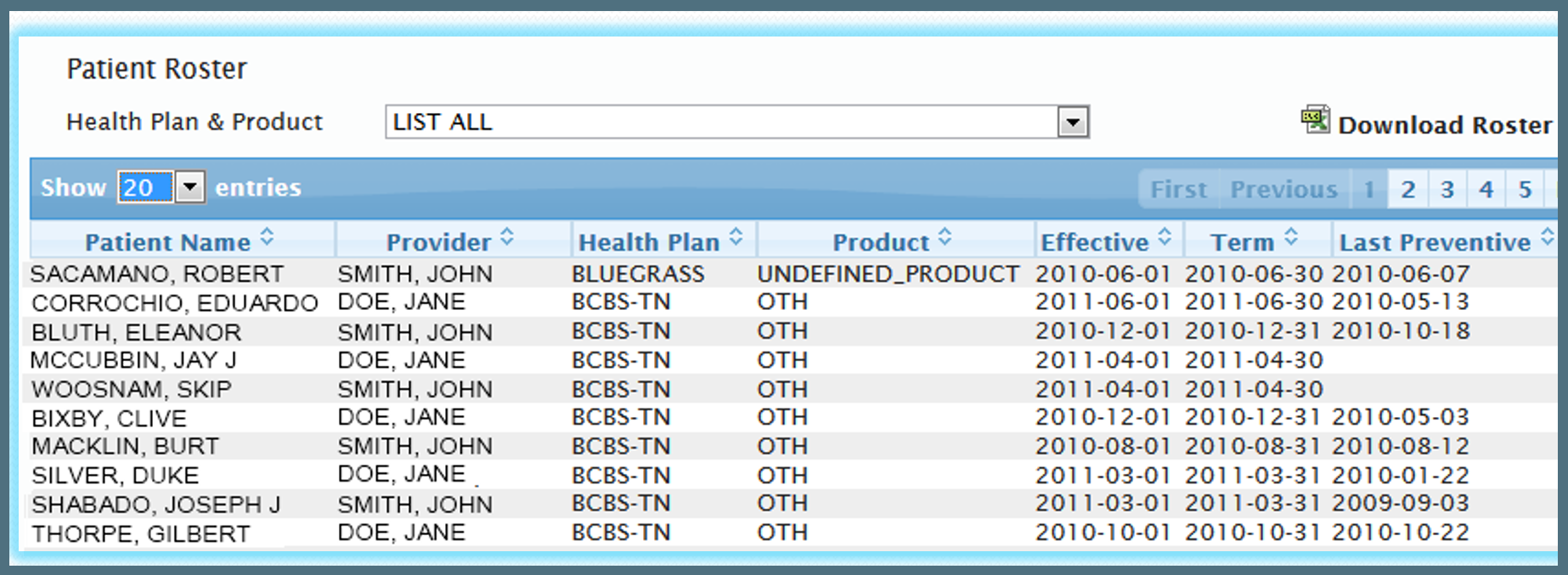
Patient Registry
Using a breakdown of HEDIS style metrics and your patient's claim and lab data, we provide reporting and other alerts to monitor patient progress. This allows providers to track data over time, highlight potential improvement areas, and monitor the success of care initiatives.
HEDIS is a set of performance measures designed to improve the overall quality of health care performance. These metrics cover a wide range of health problems such as diabetes, heart disease, and cancer.
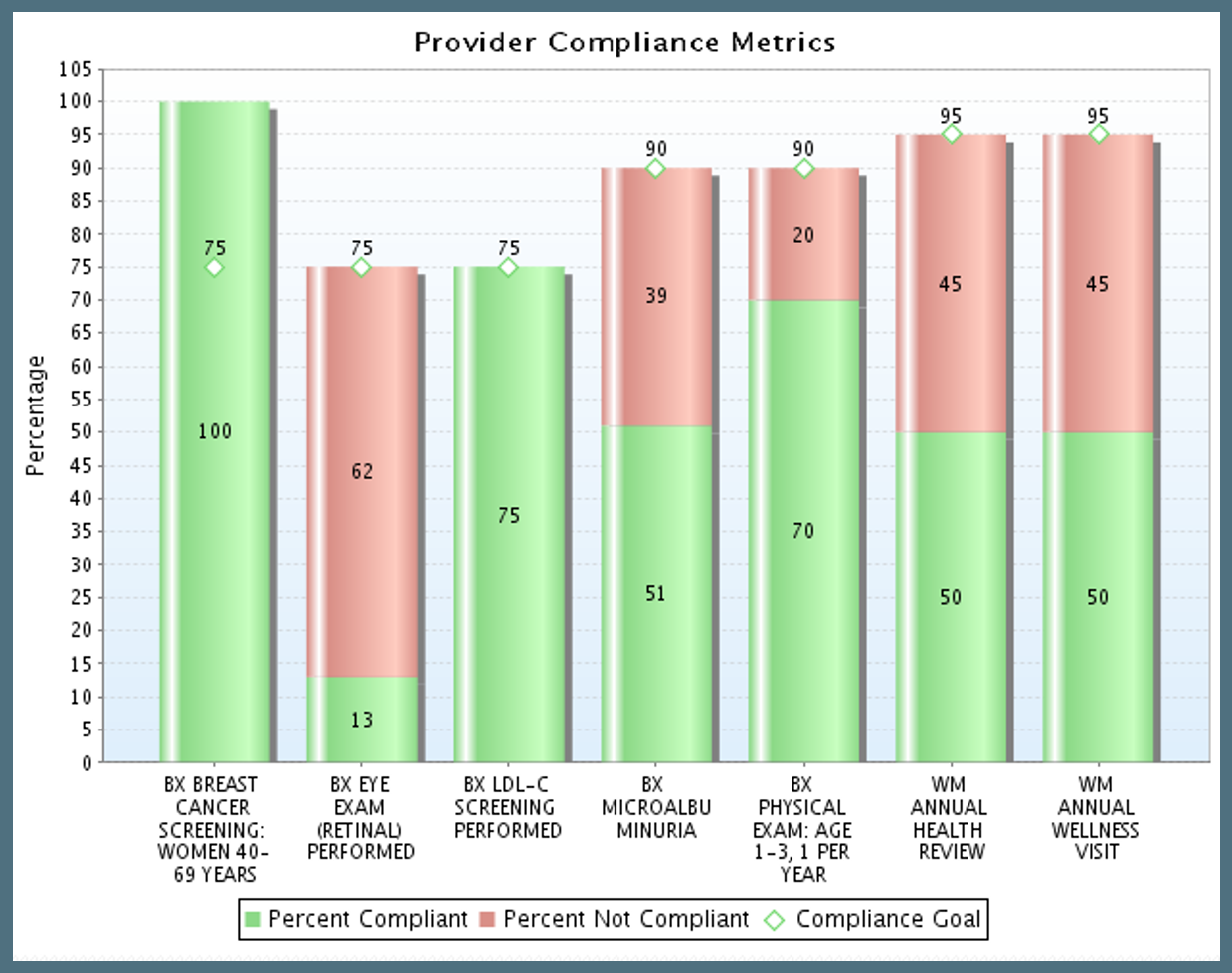
Custom Reporting
Our systems are capable of creating flat views of your data for analysis. The views are an aggregate of your claims information called "cubes" which is a quick and easy method for data extraction. We then take this data and create graphs, spreadsheets, and the PDF documents of your choice.