Claims Repricing
Many of our clients have a need to price claims based on custom contracts with both the payor and provider.
Contract Management
Our pricing tools are built in such a way to prevent repeating of the same fee schedule data over and over.
Payment Processing
Take the hassle out of tracking payments, denials, and reversals with our custom rule engine for processing 835.
ANSI EDI
We have tools to create and parse ANSI files both institutional and professional such as 837, 835, 999 and 277.
Claims Software
Claim Pricing
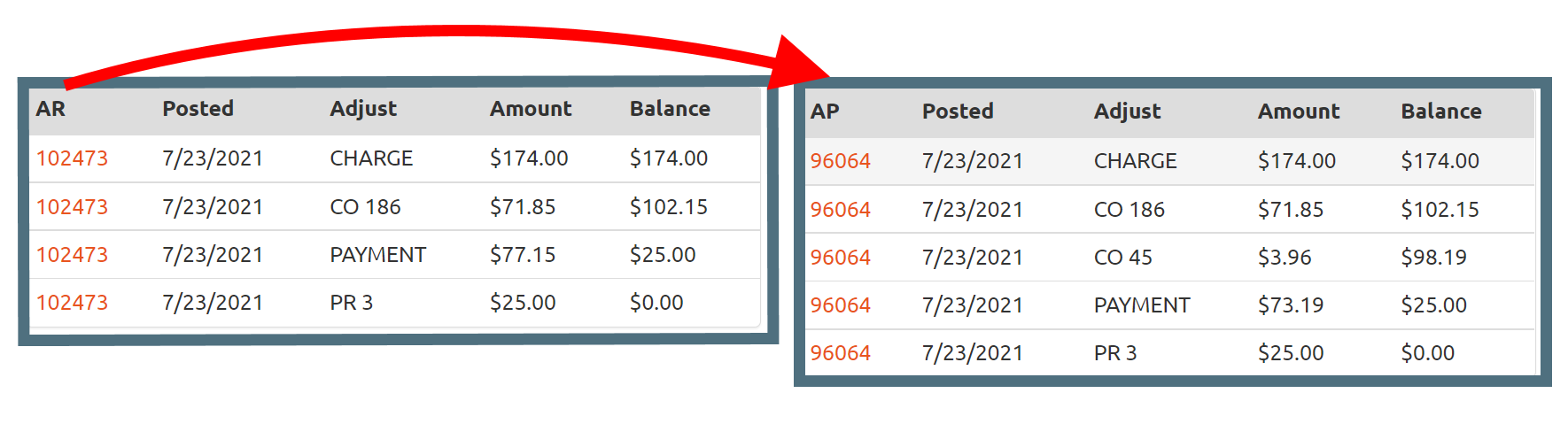
Many of our clients have a need to price claims based on custom contracts with both the payor and provider. This could be a risk based per member, per month contract or simply a fee for service based contract. Prices for claims are defined when they are received from the provider. Defining what is owed to the provider versus what the payor owes up front means that you can track both sides of your accounting with ease.
Contract Management
We create a well-defined set of rules for claims pricing and administration fees. These rules are not limited to static fee schedules. We have the capability to expand the schedule by effective and term dates, percentages, and other custom rules without the need to duplicate large fee tables for any special cases.
The contracts and fee schedules are easily managed using online tools that are able to address these common issues without making a mess of your data. The editors typically support custom contracts for fee-for-service schedules, risk based contracts, bulk import and other special case rules.
Our systems are capable of pricing claims based on DOS, strict contract amounts, billed amounts, or percentages of these amounts. We also have rules designed to handle risk or pass-through claims that need no pricing other than the ability to track what is owed in COB or patient responsibility balances.
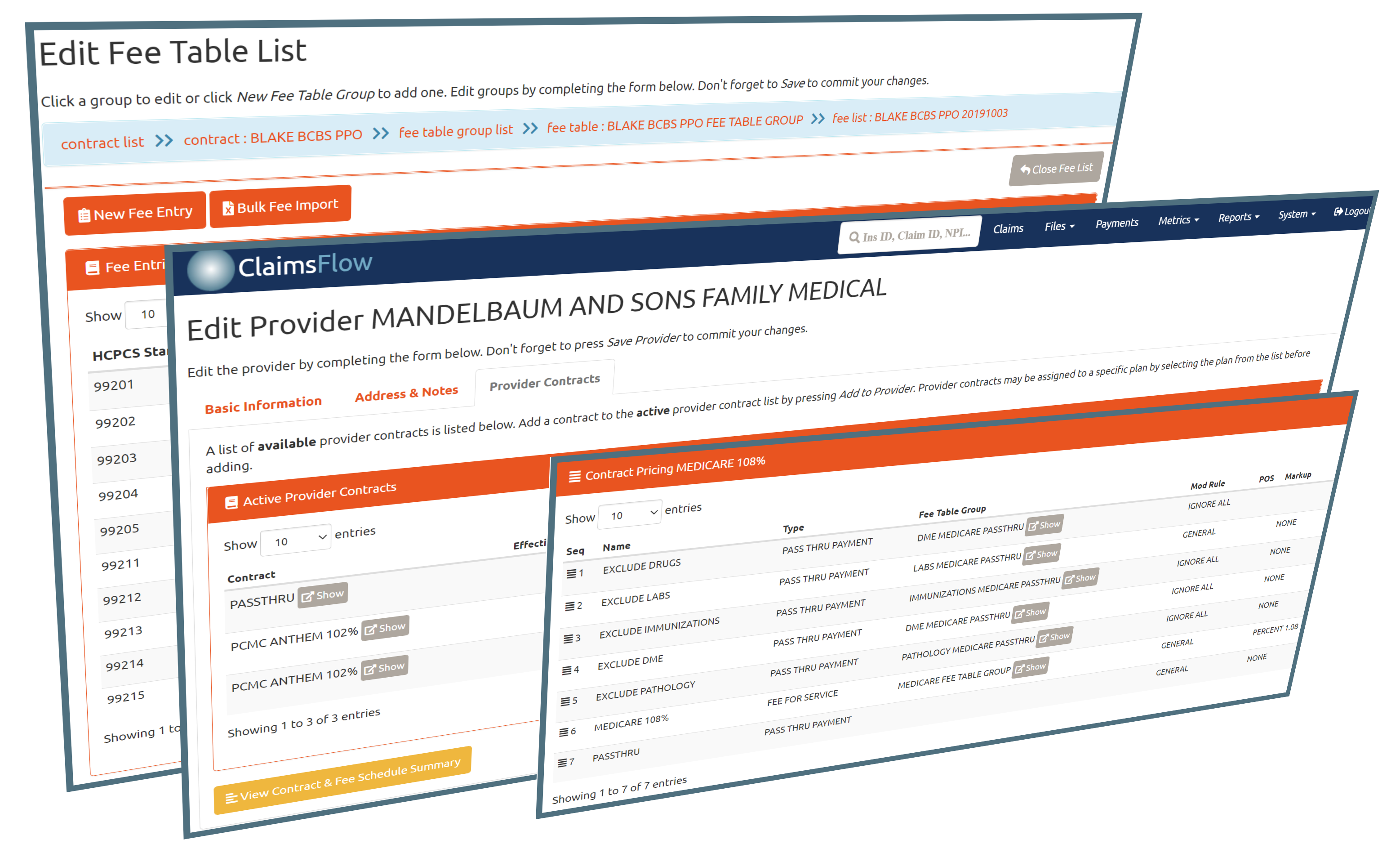
Sample Claims View
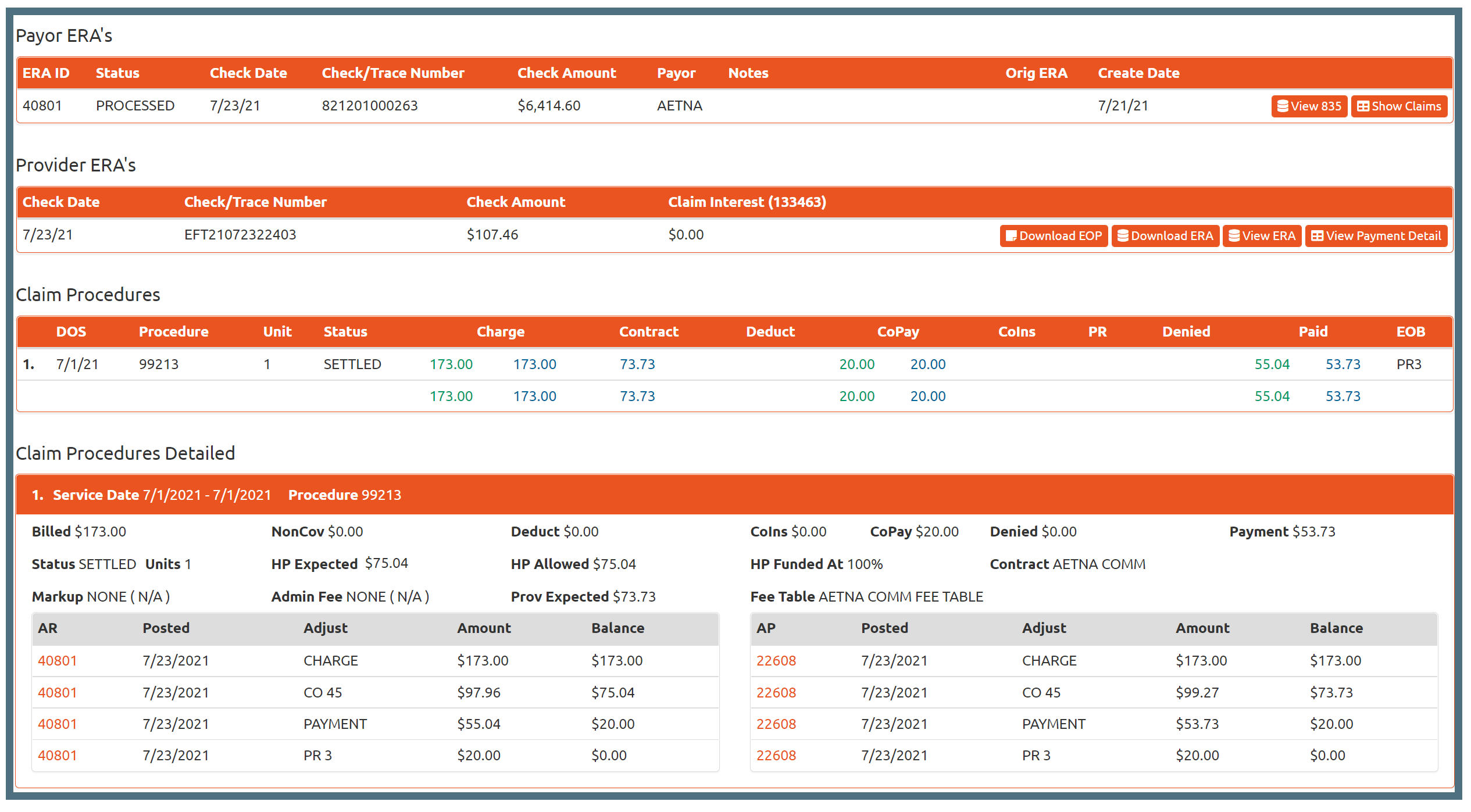
Payment Processing
Collecting and posting payment data can get complicated. For our clients, this often involves the need to track two different accounts -- one to track the what is owed from the health plan (accounts receivable, AR), and another to track what you owe the provider (accounts payable, AP).
Where some claims systems only track AR and have limited abilities in terms of paying different amounts or collecting administrative fees, our software keeps track of both AR and AP on the claim service line and can report these values easily on the web site or in billing, open AR/AP, or payment reports.
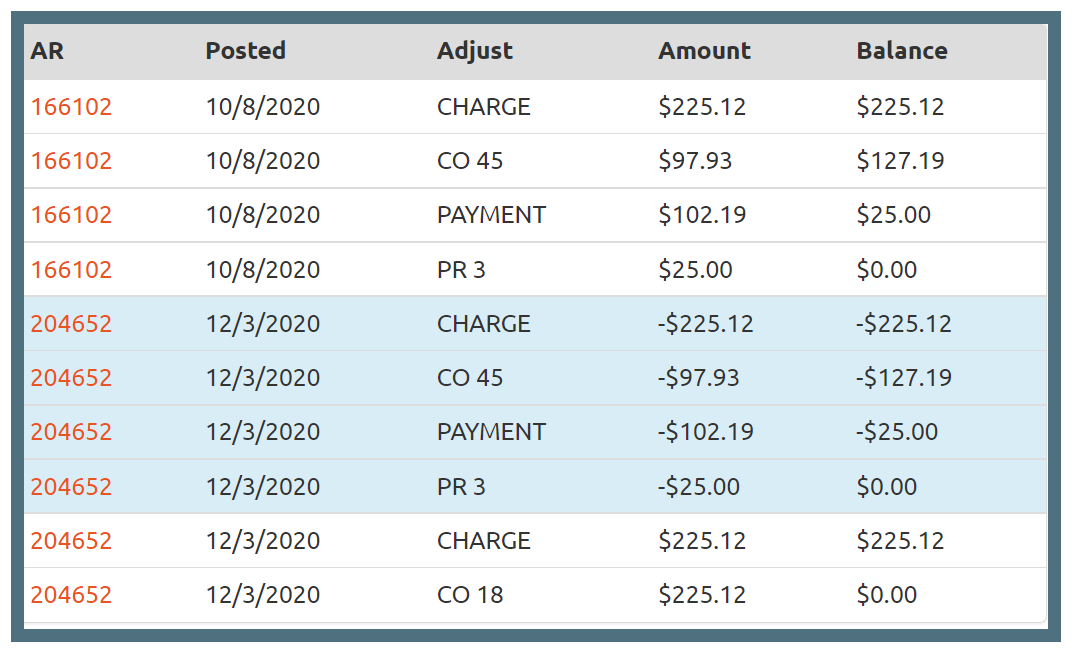
Each time a response is received from the health plan, this triggers an action on the provider payment side. If a payment is made from the health plan to AP, an equivalent payment, per the contract agreement, is made to the provider from AR. This acts as a built-in audit trail of your claim's billing and payment history. No detail is ever omitted or removed in the event of payment reversals, partial payments, duplicate payments, denials or refunds.
ANSI EDI
We have experience creating and parsing ANSI EDI files such as 837, 835, 277 and others. We are able to parse the received claims into the system for tracking and reporting. We then have the ability to take the same claims and automatically build a separate 837 file with your claim/account numbers and contracted pricing. This includes the ability to split, combine, or supplement claims as needed.
It's also possible to automate tasks using data found in 270/271 member status and 276/277 claim status reports from the health plan. These tasks can help resolve issues in a timely manner instead of waiting for a denial in an 835.
Our claim tools can display EDI in a human readable fashion. Easily identify loops and segments in popover text to see how that field is defined. Try clicking a field on the left to view ANSI details for that loop and segment.
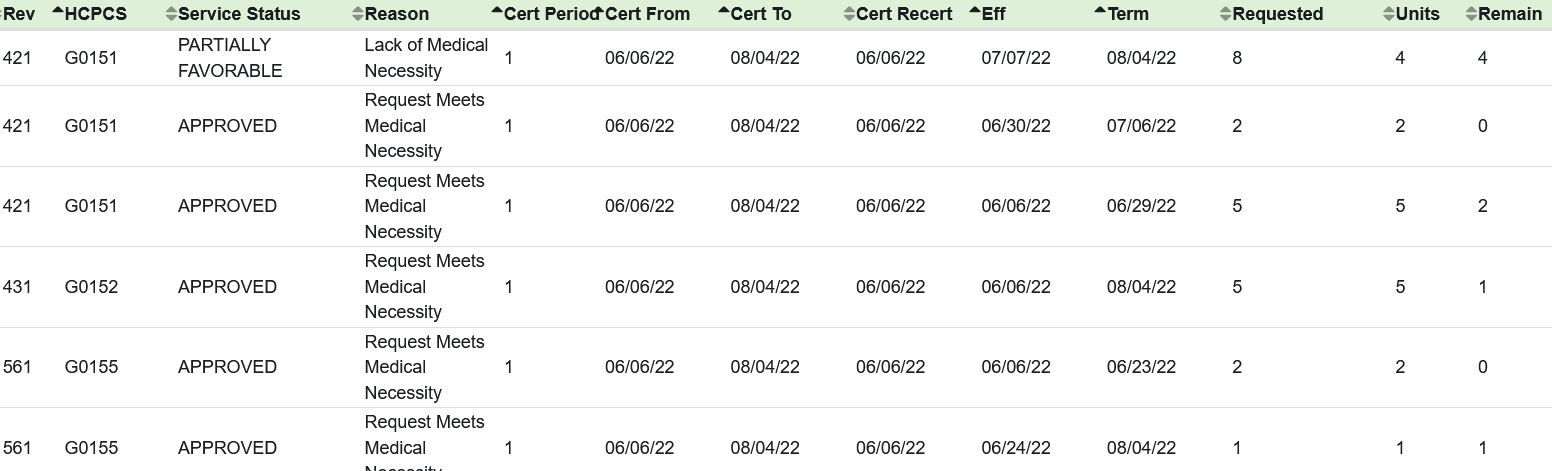
Intake, Appeals, & Authorization
Authorization tracking and utilization management are key parts of our software. The system is capable of tracking units and applying advanced logic for matching claims and claim lines.
We have experience creating customized queuing systems to handle intake. This software divides work automatically to teams of employees capable of handing certain tasks. A simple flowchart is used to manage queues and update them in real-time. This software logs all action items on the queue and can make suggestions for automation given certain inputs.
Intake, appeals, and authorization systems that are aware of each other are key to automating as much as possible. Our systems are designed from the ground up with this goal in mind.
Automation
It's common practice to automate the exchange of claims files with a health plan or clearing house. We take this a step further and automate any daily tasks that can be defined by a series of rules.
The schedule is configurable and contains an email notification system so you can easily supervise your automated tasks. This ensures that the health plan is never waiting on you to respond to denials or payments.
Being able to have a centralized place to collect and manage claims files can reduce turn-around times for your claims business. We can also provide this service as an addition to an existing claims or practice management system.
